|
Reviewed by
John K. Fink, M.D.,
SPF Medical Advisor
Index:
What
is HSP?
What is (Apparently
Sporadic) Spastic Paraplegia?
What
are the symptoms?
How
severe will my symptoms get?
What
is complicated HSP?
How
is HSP diagnosed?
What
genetic testing is available?
What
is the life expectancy?
What
is the treatment?
What
is the risk of getting HSP?
How
does HSP cause symptoms?
What other conditions cause
spastic paraplegia?
Other
Questions
Where can I get more information?
What is HSP?
HSP is a term for a group of rare, inherited neurologic disorders
along the motor neuron disease continuum. Their primary
symptom is progressive spasticity (stiffness) and weakness
of the leg and hip muscles. There are at least
twenty types of HSP and the genetic causes are known
for eleven. The disorder is estimated to affect
some 20,000 people in the U.S.
There are many different names used for HSP. The most
common are Hereditary Spastic Paraplegia (or Paraparesis),
Familial Spastic Paraparesis (or Paraplegia) and Str�mpell-Lorrain
Disease. Others are Spastic Paraplegia, Hereditary Charcot-Disease,
Spastic Spinal Paralysis, Diplegia Spinalis Progressiva,
French Settlement Disease, Troyer syndrome and Silver
syndrome.
Here's a very quick overview
Chart.
Back
to Index
What is (Apparently
Sporadic) Spastic Paraplegia?
Many individuals with all the signs and symptoms of
HSP do not appear to have similarly affected family
members. In these cases, some neurologists call the
condition Spastic Paraplegia or Apparently Sporadic
Spastic Paraplegia rather than Hereditary Spastic Paraplegia.
Other clinicians may diagnosis the same condition as
Primary Lateral
Sclerosis, which mimics HSP but over time,
eventually also involves the arms and speech and swallowing
muscles as well as the leg muscles.
There are many reasons why someone with HSP may not
have a family history. Recessive and x-linked forms
skip generations, which means the disorder may pass
down silently for generations and then suddenly appear.
Additionally, there is wide variability in age of onset,
progression rate and severity so that the disease may
have been undiagnosed or someone may have passed away
prior to symptom onset. There is also the possibility
of mistaken parentage, or, that a new mutation has occurred.
Please see HSP
and Heredity.
Back
to Index
What are the
symptoms?
The hallmark symptom of HSP is progressive difficulty
walking due to increasingly weak and taunt (spastic)
muscles. Most people have symptom onset between the
second and fourth decades of life, but it can start
at any age from early childhood through very late adulthood.
Initial symptoms are often difficulty with balance,
stubbing the toe or stumbling. Often, changes begin
so gradually that other people notice the change first.
As the disease progresses, canes, walkers and eventually
wheelchairs often become needed, although some people
never require assistive devices. There can be a great
deal of variability in severity of symptoms and age
of onset, even within the same family.
Other symptoms that commonly occur are urinary urgency
and frequency, difficulty with balance, hyperactive
reflexes, clonus, Babinski's sign, diminished vibration
sense in the feet, muscle spasms, pain and pes cavus
(high arched foot). Sometimes, urinary disturbance is
the first symptom. A good portion of people report
painful spasms and other pain. (Editor's Note: One of
our community members, who is a primary care physician
with HSP, has submitted an article about pain
management. Please see
Articles - Pain.)
The majority of people with HSP have �uncomplicated�
HSP, as described above. There are also rare, "complicated"
forms, which involve additional symptoms such as peripheral
neuropathy, ichtyosis (a skin disorder) epilepsy, ataxia,
optic neuropathy, retinopathy, dementia, mental retardation,
deafness, or problems with speech, swallowing or breathing.
However, existence of these symptoms may be caused by
other reasons. For example, someone with uncomplicated
HSP may have peripheral neuropathy caused by diabetes
or could have epilepsy for unrelated reasons.
Back
to Index
How
severe will my symptoms get?
There is no way to predict rate of progression or severity
of symptoms. Generally, once symptoms begin, progression
continues slowly throughout life. For some childhood
onset forms, however, symptoms may become apparent,
gradually worsen, and eventually stabilize after adolescence.
HSP rarely results in complete loss of lower limb mobility.
Back
to Index
What is Complicated HSP?
"Complicated" HSP is a term for conditions of HSP
that involve neurological impairments in addition to
progressive spasticity and weakness of the the affected
muscles. These
include optic neuropathy, retinopathy (diseases of the
retina), dementia, ataxia (lack of muscle control),
icthyosis (a skin disorder resulting in dry, rough,
scaly skin), mental retardation, peripheral neuropathy,
and deafness.
Back
to Index
How is HSP
diagnosed?
Diagnosis is a made through a careful clinical examination,
a process of exclusion of other disorders causing progressive
spasticity and weakness in the legs and an observation
period to see if other symptoms develop that indicate
another condition. Disorders that can be ruled out with
testing are ALS, tropical spastic paraparesis (TSP),
vitamin deficiencies (B12 or E), thoracic spine herniated
disks, and spinal cord tumors.
HSP is hereditary, and examining family history is
important in diagnosing HSP. However, many individuals
with all the signs and symptoms of HSP do not have a
family history. See (Apparently
Sporadic) Spastic Paraparesis.
Genetic testing for the most common form of dominant
HSP (spastin) and for the most common form of childhood
onset dominant HSP (atlastin) is available.
Back
to Index
What
genetic testing is available?
Athena Diagnostics offers testing for mutations
in the SPG4/spastin gene, the most common form of dominant
HSP. The test is called the Hereditary Spastic Paraplegia
Evaluation and costs approximately $2000. Testing for
the SPG3A/atlastin gene, the most common childhood-onset
form, has just been announced as available. As more
genes are discovered, it is hopeful that such information
will lead to greater availability of testing.
Genetic counselors can be found at many major medical
centers or by contacting the National Society of Genetic Counselors
at (610) 872-7608. Gene tests can be used for prenatal
testing.
Back
to Index
What
is the life expectancy?
Life expectancy is normal. However, complications
arising from falls or immobility caused by the symptoms
of HSP may inadvertently shorten a person's life.
Back
to Index
What is the
treatment?
There is currently no treatment to prevent, stop,
or reverse HSP. Treatment is focused on symptom relief,
such as medication to reduce spasticity and other symptoms;
physical therapy exercise to help maintain flexibility,
strength, and range of motion; assistive devices and
communications aids; supportive therapy and other modalities.
For detailed information about treatment and therapies,
click
here.
Back
to Index
What
is the risk of getting HSP?
There are at least twenty different forms of HSP, and
there are three different modes of inheritance: autosomal
dominant, autosomal recessive and X-linked. Each mode
has a different risk factor, which ranges from almost
none to 50%. For detailed information, please click
Heredity and HSP.
Back
to Index
How
does HSP cause symptoms?
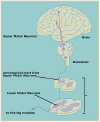 HSP
is caused by degeneration of the upper
motor neurons in the brain and spinal cord. Upper
motor neurons control voluntary movement. HSP
is caused by degeneration of the upper
motor neurons in the brain and spinal cord. Upper
motor neurons control voluntary movement.
The cell bodies of these neurons are located in the
motor cortex area of the brain. They have long,
hair-like processes called axons that travel to the
brainstem and down the spinal cord. Axons relay the messages to
move to lower motor neurons that are located
all along the brainstem and spinal cord. Lower motor
neurons then carry the messages out to the muscles.
Click on the diagram at right to see how upper motor
neurons connect to lower motor neurons that innervate
leg muscles.
When upper motor neurons degenerate, the correct messages
cannot reach the lower motor neurons, and the lower
motor neurons cannot transmit the correct messages to
the muscles. The result is increased muscle tone (spasticity)
and weakness. As the degeneration continues, spasticity
and weakness increases. The legs are affected because
degeneration occurs primarily at the ends of the longest nerves
in the spinal cord, the ones that control the legs. In
some cases, the upper body can be minimally affected as
well, leading to problems with arm or speech and
swallowing muscles.
Back
to Index
What
other conditions cause spastic paraplegia?
Spastic paraplegia symptoms can also be caused by
other conditions. A virus-caused disease with symptoms
similar to HSP is
Tropical Spastic Paraparesis.
Disorders with spastic paraplegia symptoms termed Lathyrism
and
Konzo are caused by
toxins in the plants Lathyrus sativus and cassava.
Other causes of spastic paraplegia include (but are
not limited to) primary lateral sclerosis, spinal cord
injury or tumors, cerebral palsy, multiple sclerosis,
amyotrophic lateral sclerosis, vitamin absorption issues,
and thoracic spine herniated disks.
Back
to Index
Are foot problems common?
Yes. Here are some common foot problems:
-
High arched feet (pes cavus). High arches
occur because there is more weakness in the foot
muscles that extend the foot backward and flatten
the arch than in the muscles that flex the foot
downward.
-
Shortened Achilles tendons. Achilles tendons
are often short, and generally shorten further as
HSP progresses.
-
Jumping feet (clonus). Clonus is an uncontrollable,
repetitive jerking of muscles that makes the foot
jump rapidly up and down. It occurs when the foot
is in a position that causes a disruption of the
signals from the brain, leading to an automatic
stretch reflex.
-
Hammer toes or bunions. These may occur
due to imbalances in the strength and tone of muscles
that maintain proper alignment of joints in the
feet.
-
Cold feet and/or foot swelling. This is
most likely caused by poor circulation. Normally,
muscle contractions in the legs help pump blood
from the legs back to the heart. If the muscles
are weakened, or if the person is relatively inactive,
the blood flow from the legs may be decreased, and
fluids may accumulate. This can cause swelling,
or a sensation of "cold feet".
Back
to Index
Can my arms get affected?
Some people may experience problems with their
arms or fine motor control of their fingers. The
degeneration in nerves that supply the arms is mild
compared to that which occurs in the nerves that supply
the legs. For most people, this is not significant.
Back
to Index
Is depression normal?
Periods of feeling down about having HSP are normal
and expected. It is not uncommon for people to also
experience periods of clinical depression.
Back
to Index
Why are my symptoms different from others?
There is enormous variability in age of onset, progression
rate and severity of symptoms in HSP. One reason is
that HSP is a group of genetically different disorders,
not a single disorder. Some differences may be due to
having HSP caused by different genetic mutations.
However, symptoms can also differ widely among family
members with the same gene mutation. A child may show
symptoms before a parent and it�s possible for some
family members to have very mild symptoms while others
have more severe symptoms. This may be due to factors
such as other genes, environment, nutrition, general
health, or and other factors not yet understood.
In some families, symptoms tend to start at younger
ages with each new generation. Although it is rare,
HSP sometimes shows �incomplete penetrance�. This means
that occasionally, an individual may have the gene mutation,
but for unknown reasons never develop symptoms of HSP.
Such individuals can still pass HSP down to children.
Back
to Index
Why are my muscles tighter when I am stressed?
Many people find the tightness in their muscles worsens
when they are angry, stressed, or upset. It is unknown
exactly how emotions affect muscle tone, but it may
involve adrenalin levels.
Back
to Index
Can HSP affect sexual function?
The short answer appears to be "yes", although it is
important to remember that sexual desire and/or function
can be affected by many other factors such as older
age, stress, depression, fatigue, medical disorders
or medications.
Some people report that stiffness, spasms and cramps
that are part of HSP may either inhibit (or intensify)
orgasm, or that orgasm may bring on leg stiffness, spasms
or clonus. Stiffness of the legs may cause difficulty
using certain positions for intercourse.
Back
to Index
Is HSP an Ataxia?
No. The group of disorders known as Ataxias (such as
Friedreichs Ataxia) are spino-cerebellar disorders in
which there is a disturbance either in the part of the
brain known as the cerebellum or in the connections
to it. HSP does not involve the cerebellum. Ataxias
can be hereditary or sporadic.
The term "ataxia" means incoordination, and can also
refer to a symptom in which there is a lack of muscle
control resulting in a jerky or unsteady movement. People
with HSP may have incoordination as a symptom. This
does not mean they have Ataxia.
Back
to Index
Can I donate blood?
HSP cannot be passed to others through donation of
blood. There is no medical reason why a person with
HSP cannot donate blood.
Back
to Index
When was HSP identified?
In the late 1800's, A. Str�mpell, a neurologist in
Heidelberg Germany, described this disorder. He observed
two brothers and their father, who had gait disorders
and spasticity in their legs. After the death of the
brothers, Str�mpell was able to show through autopsy
the degeneration of the nerve fibers leading through
the spinal cord. The disorder was originally named after
Str�mpell, and after two Frenchmen who later provided
more information about the disorder, Lorrain and Charcot.
Back
to Index
Is HSP more prevalent in certain ethnic groups?
There is no evidence that HSP is more prevalent in
one ethnic group than another.
Back
to Index
Please visit
Information to get a listing of articles
you can download from the Internet or order from the
SPF.
Back
to Index
|








